Selected projects
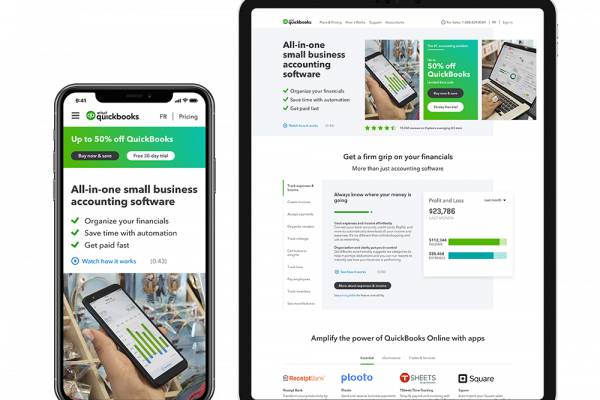
QuickBooks
PRODUCT SELECTOR
Designed UX experience to help customers choose the right package for their accounting needs.
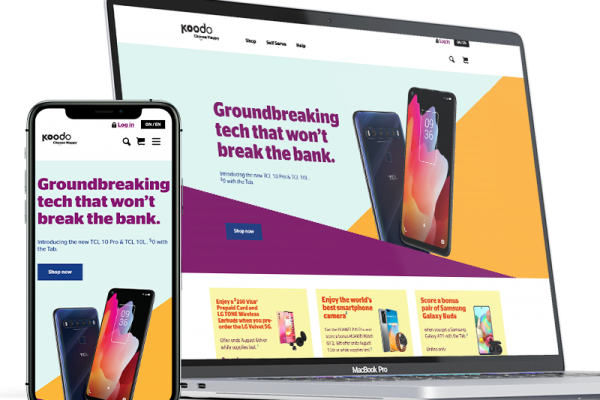
Koodo
2 Step Authentication
Designed UX flow to stop online fraud orders.
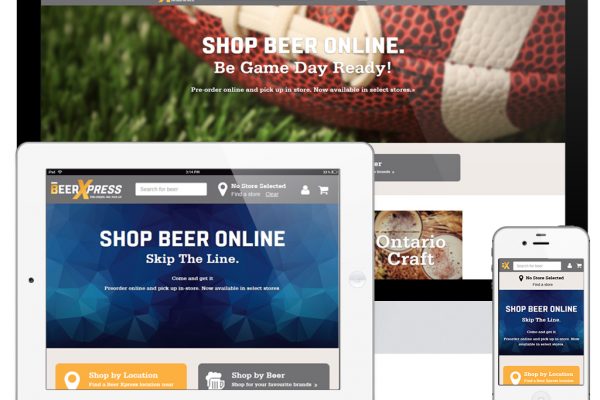
BeerStore
Beer Xpress App
Designed entire eCommerce website, iOS, and Andriod app.
About me
I am Dhaval Naik, UI/UX and interactive designer based in Toronto, Canada. When working on a new design I always try to create eye-catching visuals that strongly convey the message of the products and services that are being offered to the users. This involves careful planning, meticulous competitive analyzing, storyboarding, creating multiple mock-ups that eventually leads to a rich user experience design.
Having more than 10 years of hands-on experience in designing applications for iOS, Android, B2C and B2B websites, web-apps or just simple websites. Produce end-to-end user experience by ensuring that I am incorporating user-centered design techniques, and optimize the experience.
After completing a course in 3D Modeling and Visual effects at Humber College, I am taking my creative ideas to a new perspective.
If I am not designing or coding, I will be either spending time with my family or taking photos on my Canon DSLR.
- UI/UX Design for iOS and Android smartphones and tablets
- Design responsive web-apps and websites using HTML5 & CSS3, Bootstrap, Javascript and jQuery
- Design and develop responsive email templates
- Design a rich multimedia presentation using Adobe After Effects and Flash
- Create/design icons for apps and websites
- Experience in advertising, SEO, SEM and Google Analytics
- Design print materials such as brochures, magazines, and posters
- Identity design including logos, stationery, and branding
- 3d modeling and visual effects
- Environmental graphic design such as signage systems and exhibits



